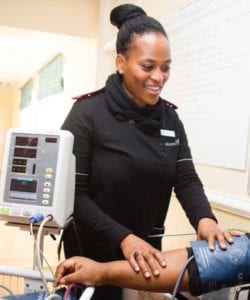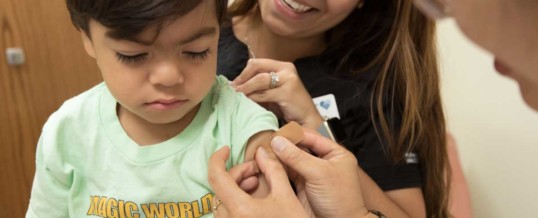
People on the autism spectrum visit emergency departments far more often than the average person and usually get worse service and outcomes.
Individuals with autism are largely given the same treatment as everyone else despite their sensory and perceptual differences, which typically leads to predictably bad outcomes for both the patients and the Emergency Departments, potentially endangering lives.
When Appendicitis is Mistaken for Common Stomach Pains
For example, one patient with autism that came into an emergency department with stomach pains was discharged only to come in the next day with a ruptured appendix. Why was this missed?
The doctors didn’t understand that due to his autism he perceived pain differently, so despite having appendicitis he was misdiagnosed with stomach pains and he was discharged when he should have had surgery.
Instead, he returned the next day after his appendix ruptured to get surgery.
If it would have been properly diagnosed the day before the surgery could have been done before the appendix ruptured and had the chance to infect other internal organs.
Open surgery is almost always required after an appendix has ruptured in order to ensure all infected areas are treated, which has a 2-4 week recovery time. If it was caught beforehand they could have used laparoscopic surgery which is less invasive and has a 1-3 week recovery time.
“A study in the Journal of the American College of Surgeons found the risk of rupture was less than 2 percent when appendicitis was treated within 36 hours of the start of symptoms. It increased to 5 percent when it was treated 36 hours or more after the start of symptoms.”
Understanding that there are people who will experience the same symptoms at a very different degree or in a different way is extremely important to properly diagnosing things like appendicitis where every hour it goes untreated puts the patient at greater risk for something significantly more severe.
 Understanding the Differences in Pain Perception is Important
Understanding the Differences in Pain Perception is Important
It is important for non-medical staff and medical staff alike to understand how someone with autism can respond differently so they can make a number of small changes in their approach that can make a huge difference in the effectiveness of diagnosis and treatment for patients across the autism spectrum.
Here are two more in depth stories to show how things can go wrong when someone on the autism spectrum visits the emergency department and their needs aren’t properly understood.
Stoicism and Lack of Expression of Pain Lead to Misdiagnosis and Delay in Treatment
Cheryl could tell from changes in his mannerisms that Dominique had not been feeling well, but once he actually told her that something was wrong she knew it was bad.
Dominique has an abnormally high pain tolerance due to his autism. Normally when he bothers to say something is wrong, it is quite serious.
Cheryl took Dominique to the nearby emergency department where her family was visiting in Rhode Island in the middle of the night.
This particular emergency department had people from the nearby jail come in during the middle of the night. The security guard and crowd of people put Dominique even more on edge than the ED normally would. He already had communication challenges due to his autism, but each thing that adds extra stimulation makes it less likely of having a successful visit. The extra noise and crowd had him in a heightened state of awareness while in the waiting room.
What Happens at Intake is Crucial for the ED Experience with Autism
Cheryl tried to communicate with the front desk staff that her son has autism and that he would act differently than a typical child of his age, but they didn’t know what that meant. By the time Cheryl and Dominique were being treated by medical staff Dominique was at the edge of overwhelm and not very responsive to the medical staff.
Due to Dominique’s stoic demeanor and lack of clearly expressing or communicating the pain, the medical staff did not think anything serious was wrong with him. The medical staff were further overwhelming him, causing him to withdraw even more. They didn’t understand his sensitivity to touch or that slowing down would be helpful for him to feel more comfortable.
He no longer wanted to communicate, leaving Cheryl hard pressed to communicate what was wrong.
The doctor didn’t think he was that sick so he was discharged.
The next day Cheryl had to bring him back to the same Emergency Department and he was diagnosed with pneumonia and a double ear infection.
Challenges with Nonverbal Autism and Communication
Sarah brought her child into the children’s ER in Jacksonville. She had already been to her son’s primary care physician and he had sent her to the children’s ER for further testing. Due to her son not favoring the body parts that were hurting and the nonverbal nature of her child, his symptoms were largely dismissed.
Her son’s low energy levels and lack of eating were also deemed to not be of significant enough concern. This was day 12 of a low grade temperature.
It took another 6 weeks of doctors appointments before finding out that the child had strep throat.
This is something that could have been treated much earlier on if his autism had been more thoroughly understood, leading to both understanding the range of possibilities of what could be wrong with the child as well as understanding the context of the concern of the parent better.
In many cases the caretaker for someone with autism is going to be the best insight into what is normal for that child or adult. Autism by nature varies significantly by person, so just because a doctor has seen numerous patients with autism that does not mean that a new patient will be similar to previous patients.
This is one of the biggest reasons why proper training on autism is so important across medical and non medical staff alike. Autism is a spectrum, and how people are treated needs to reflect that.
Where do Emergency Departments Need to Improve?
Each step of the process through an emergency department is a chance for escalation or de-escalation on a sensory level for someone with autism.
If the staff doesn’t have training and there aren’t resources available, each step of the process will likely escalate the person with autism’s sensory state and get them closer to a meltdown, oftentimes making treatment very difficult if not impossible.
Many times this forces the patient to come back for something that could have been more effectively treated the first time, like in Cheryl’s case with her son Dominique. Other times they don’t get treatment at all because a combination of factors lead to them getting overwhelmed and having a meltdown, making treatment too challenging for the medical staff.
Overlooking Sensory Differences can Lead to Lack of Viable Treatment
This is what happened when Cheryl brought in her 2 year old daughter with a 104 degree fever. The medical staff were not mindful of the child’s sensory differences when trying to give her an IV of fluids, overwhelming her to the point where she would resist and flail every time they tried to get the IV in. This lasted for an hour and a half before they decided it was more traumatic to continue than it was worth for the benefit of the IV and discharged her without treatment.
If the nurse would have better understood the differences of someone with autism this could have been prevented. Oftentimes patients with autism are well on their way to overwhelm before they get to see medical staff but none of the staff are even aware of it.
Most nurses and doctors do not know what types of things will be potentially triggering for an individual on the spectrum or what to look out for, leaving whether or not they escalate the arousal levels of that person purely up to chance and potentially compromising their care in the process.
 What Medical Staff Often Don’t Understand
What Medical Staff Often Don’t Understand
Most medical professionals don’t understand how important it is to be aware of the sensory, perceptual, and communication differences of someone on the autism spectrum and how it can significantly impact the way they should be approached, diagnosed and treated.
There are a lot of small things that can be done throughout the process, and learning to do them is all the more important as the prevalence of autism continues to grow. Based on a recent study by CDC, 1 in 44 children is being diagnosed with autism in the US, up from 1 in every 150 children being diagnosed in 2000.
People with autism visit the emergency department far more often than neurotyipcal people, which is why it is so important for EDs to have proper training.
These people are already visiting your ED whether you know it or not, but many people with autism (or their families) choose not to disclose their autism due to thinking it may adversely impact their care due to making false assumptions based on stereotypes and not true understanding of how different each individual with autism is.
Many of these families that choose not to disclose choose not to because of bad experiences with medical professionals in the past who did not properly understand autism.
For many parents with a child on the spectrum, whether or not to disclose that their child is on the spectrum is taken on a case by case basis. If a family knows that your staff has training in autism they can feel confident to disclose their child has autism and to know that your staff will be open to understanding the challenges of your individual child’s experience.
Many people in healthcare are surprised to learn about how extensive the bad experiences are for individuals with autism and their families due to misunderstandings and preconceived notions.
For many people on the autism spectrum and their families trust in the healthcare system is earned, not given. Make sure your staff is prepared to earn their trust.
To Find Out More About Becoming a Certified Autism Center™
Fill out the form below to learn more about our CAC Program, which includes staff certifications, training options and center certification.
JUN